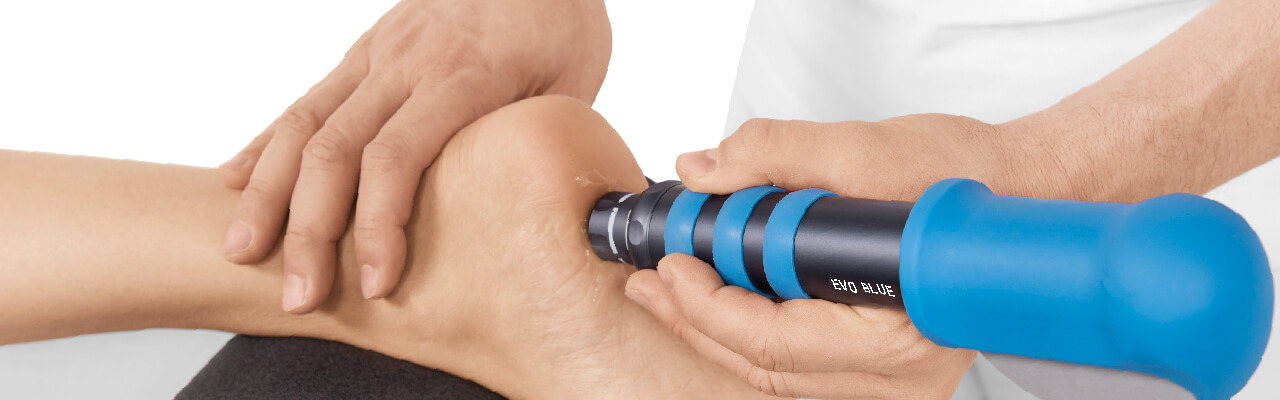
Plantar fasciopathy
Pathology
It is the most common cause of plantar heel pain and accounts for approximately 11-15% of foot symptoms presenting to physicians. The main clinical symptom is heel pain, particularly in the morning or after a period of rest. Often patients report improvement of pain after walking. Pain is usually located at the origin of the plantar fascia, i.e., at the medial calcaneal tubercle. Passive dorsiflexion of the toes may aggravate the pain in some patients, particularly in those with chronic PF. Patients suffering from chronic PF may also present with heel pad swelling.
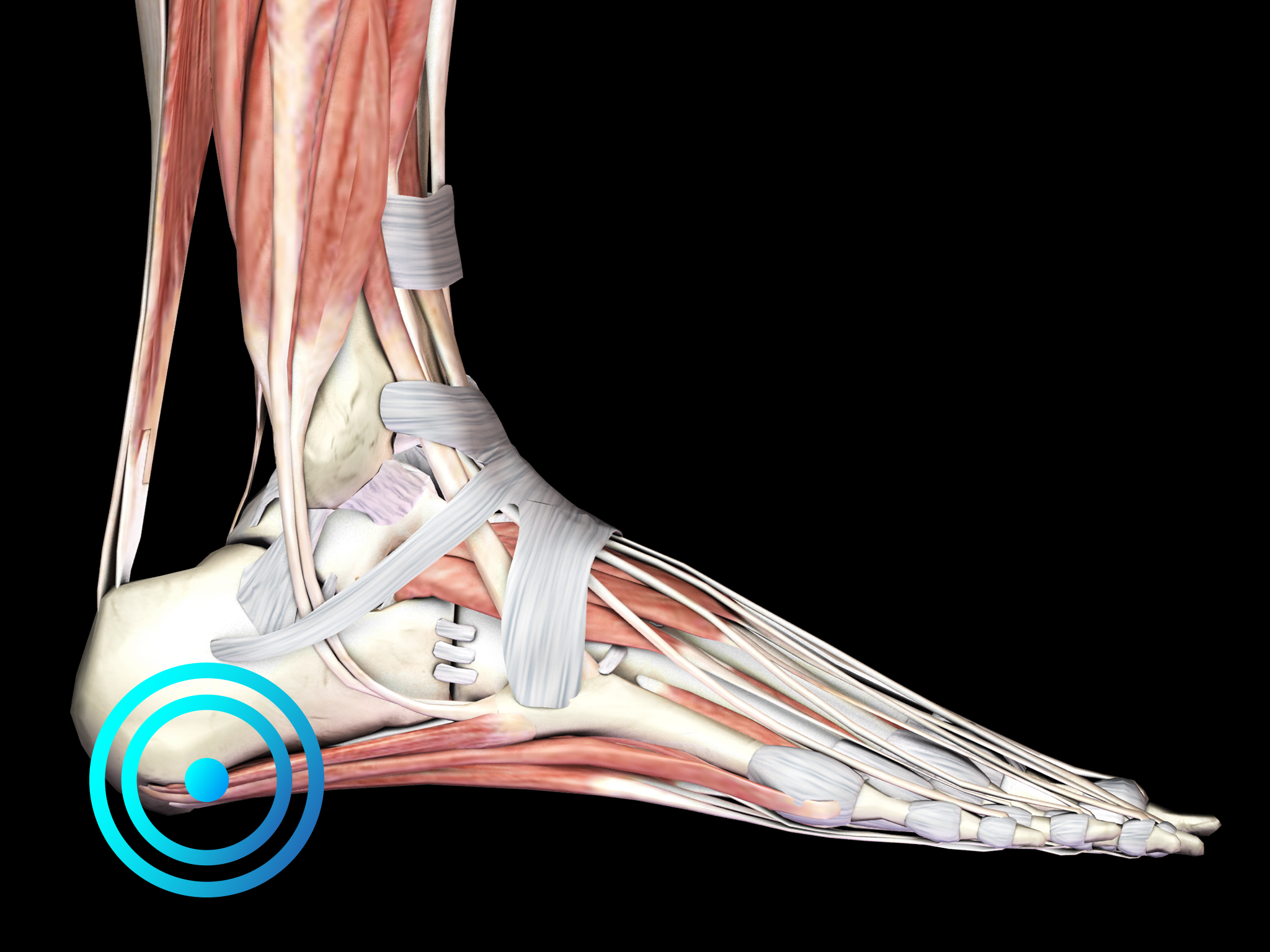
Diagnosis is based on the clinical features of the disease. Diagnostic imaging should be considered to rule out other causes of plantar heel pain or to establish the diagnosis of PF when in doubt. Histologic examination of biopsy specimens from patients undergoing plantar fascia release surgery for chronic symptoms has shown that chronic PF is associated with degenerative changes in the fascia.
Accordingly, the disease is better characterized as “plantar fasciopathy” than “plantar fasciitis”, resembling the situation in overuse tendon problems.
In the United States, more than two million individuals are treated for PF on an annual basis. Up to 10% of the population will experience plantar heel pain during the course of a lifetime.
Both athletes and the elderly commonly present to physicians with PF. The treatment of PF should start with conservative treatment modalities including rest, physiotherapy, stretching, exercises, shoe inserts/orthotics, night splints, non-steroidal anti-inflammatory drugs, and local corticosteroid injections.
Patients not responding to conservative treatment for six months (between 10% and 20% of all patients) shall then undergo radial shock wave therapy for plantar fasciopathy.
Surgery should be considered for recalcitrant cases of PF.
Side effects of Radial Shock Wave Therapy (RSWT) using the Swiss DolorClast®.
When performed properly, RSWT with the Swiss DolorClast® has only minimal risks. Typical device-related non-serious adverse events are:
- Pain and discomfort during and after treatment (anaesthesia is not necessary)
- Reddening of the skin
- Petechia
- Swelling and numbness of the skin over the treatment area
These device-related non-serious adverse events usually disappear within 36h after the treatment.
Treatment Procedure
Locate the area of pain through palpation and biofeedback.
Mark the area of pain.
Apply coupling gel to transmit shock waves to the tissue.
Deliver Radial or Focused Shock Waves to the area of pain while keeping the applicator firmly in place on the skin.
Clinical proof
Practitioner?
Get information on the diagnosis, the functioning of shock wave therapy, clinical proof, contraindications, etc.


