Midbody achilles tendinopathy
Pathology
Several terms have been used to describe this condition including tendinosis, tendinitis, and peritendinitis. However, histologic examination of biopsy specimens from patients undergoing surgery for chronic symptoms has shown that chronic MPAT is associated with degenerative changes in the tendon. Accordingly, the disease is better characterized as tendinopathy than tendinitis or tendinosis. The Achilles tendon is (together with the plantaris tendon) surrounded by a paratenon. In many cases of Achilles tendinopathy, the condition is accompanied by paratendinopathy.
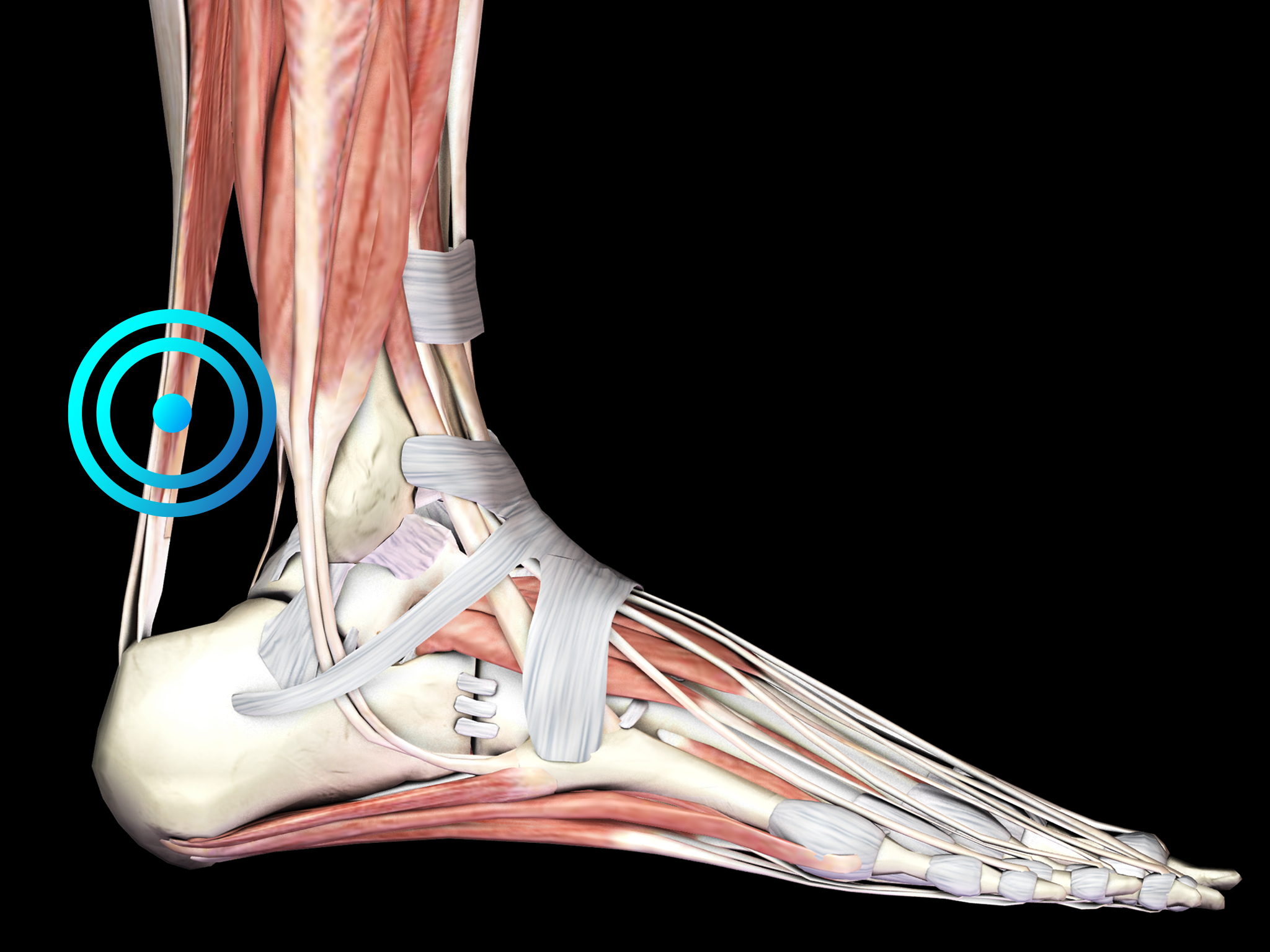
Diagnosis is based on the clinical features of the disease, with the location of the pain as an important discriminating factor. The spot of maximum pain and painful swelling in MPAT is located 2 to 6 cm proximal to the insertion, whereas in case of insertional Achilles tendinopathy, the spot of maximum pain is at the tendon-bone junction. Symptoms can be exacerbated when getting up after a period of rest. In isolated paratendinopathy, there is a local thickening of the paratenon, and the area of swelling does not move with dorsiflexion and plantarflexion of the ankle. In contrast, the area of swelling moves with dorsiflexion and plantarflexion of the ankle in case of isolated tendinopathy. Diagnostic imaging should be considered to rule out other causes of Achilles tendon pain or to establish the diagnosis of MPAT when in doubt.
As in the case of insertional Achilles tendinopathy, the aetiology of MPAT is likely multifactorial and may include advanced age, obesity, hypertension, diabetes, and steroid use, to mention only a few. Particularly in athletes, the onset of MPAT may also be influenced by poor training habits including excessive training, training on hard or sloping surfaces, and abrupt changes in scheduling.
It has been hypothesized that the healing of injuries of the Achilles tendon as a result of overuse involves the penetration of small blood vessels from the paratenon into the tendon in order to increase healing by providing improved blood flow. However, these small blood vessels are accompanied by small nerve fibres with high concentrations of nociceptive substances including glutamate, substance P, and calcitonin gene-related peptide (CGRP). Those small nerve fibres are considered the cause of pain in chronic MPAT.
The lifetime risk of an Achilles tendon injury in elite long-distance runners is approximately 50%. However, individuals of all activity levels and all ages present with similar complaints. Approximately 30% of all patients have a sedentary lifestyle.
The treatment of MPAT should start with conservative treatment modalities including rest, icing, physiotherapy, stretching (eccentric loading), exercises, orthoses, heel lifts, and non-steroidal anti-inflammatory drugs.
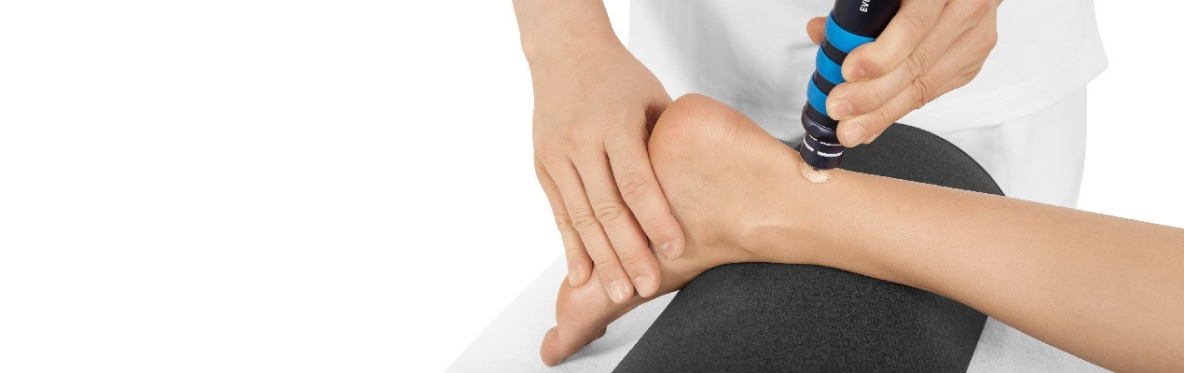
Patients not responding to conservative treatment for six months shall then be subjected to radial shock wave therapy for midbody achilles tendinopathy treatment.
Surgery should be considered for recalcitrant cases of MPAT, with different surgical strategies aiming at debridement or tenotomy of the tendon itself).
Side effects of Radial Shock Wave Therapy (RSWT®) using the Swiss DolorClast®
When performed properly, RSWT® with the Swiss DolorClast® has only minimal risks. Typical device-related non-serious adverse events are:
- Pain and discomfort during and after treatment (anesthesia is not necessary)
- Reddening of the skin
- Petechia
- Swelling and numbness of the skin over the treatment area
- These device-related non-serious adverse events usually disappear within 36h after the treatment.
Treatment Procedure
Locate the area of pain through palpation and biofeedback.
Mark the area of pain.
Apply coupling gel to transmit shock waves to the tissue.
Deliver Radial or Focused Shock Waves to the area of pain while keeping the applicator firmly in place on the skin.

